Saturday Kitchen viewers were left in tears after the BBC show paid tribute to late Hairy Bikers star Dave Myers.
The television chef died on Wednesday at the age of 66 with his friends and family at his side, two years after revealing that he was undergoing treatment for an unspecified type of cancer.
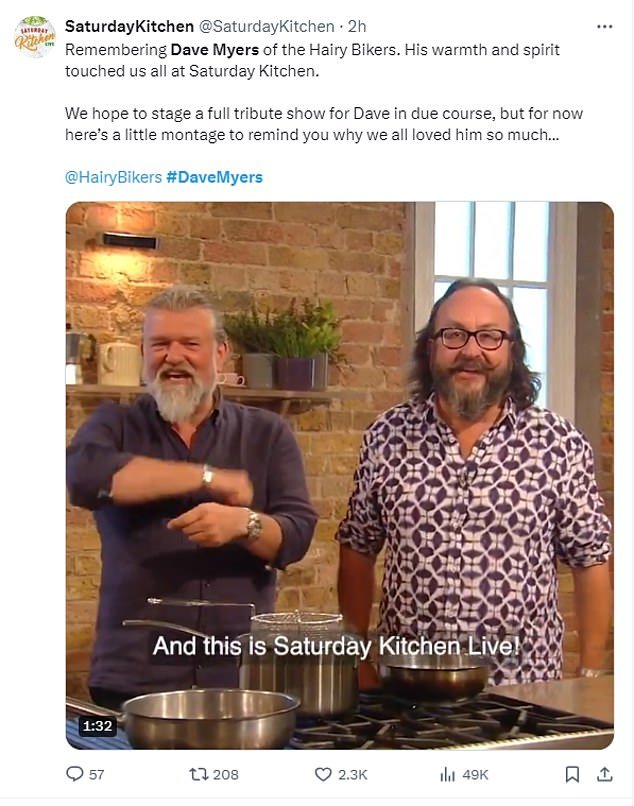
As tributes poured in throughout the week, the cooking show shared its own montage of Dave’s best parts as host Matt Tebbutt honored the star.
Speaking to the camera at the start of the show, Matt made the emotional opening speech: ‘Now, as I’m sure you know, this has been a very sad week because we lost someone very close to the program. Dave Myers, who was half of the Hairy Bikers, along with Si King.
‘They have been on the show countless times over the last 18 years and even presented it a few times. We were privileged to have Dave back in the studio last October, after he was recovering from another round of treatment.

Saturday Kitchen left viewers in tears with emotional tribute to late Hairy Biker Dave Myers


Tributes have been pouring in all week, with the cooking show sharing its own montage of Dave’s best parts as host Matt Tebbutt honored the star in an emotional speech.
Then he bravely got back on his bike and continued his TV life with Si. But unfortunately cancer took him from us too soon.”
Matt then revealed the show’s plan to air an entire show dedicated to Dave at a later date.
He continued: “We hope to put on a full tribute show for Dave in due course, but here’s a little montage to remind you why we love him so much.”
As the montage played, the BBC captured Dave’s sense of humor and abundant energy throughout his numerous appearances on the show.
In the hilarious clips, one showed Dave struggling to get pudding out of a bowl as it collapsed onto the plate.
Another saw Dave showing off his singing talent as he sang Don’t Cry For Me Argentina in a memorable episode.
Si and Dave’s strong friendship was also made clear when Dave kissed his friend on the cheek as they showed off their effortless camaraderie.
And fans were beside themselves after watching the clip as they took to Twitter to share their condolences after crying.


As the montage played, the BBC captured Dave’s sense of humor and abundant energy throughout his many appearances on the show.




In the hilarious clips, one showed Dave struggling to get pudding out of a bowl as it collapsed on the plate.


Another saw Dave showing off his singing talent as he sang Don’t Cry For Me Argentina in a memorable episode.


Si and Dave’s strong friendship was also made clear when Dave kissed his friend on the cheek as they showed off their effortless camaraderie.

Matt also revealed the show’s plan to air an entire show dedicated to Dave at a later date.






Fans were beside themselves after seeing the clip as they took to Twitter to share their condolences after crying.
One wrote: “I don’t cry at 10 in the morning,” while a second gushed: “I laughed and cried all at the same time.” Very sad.’
A third wrote: “A lovely tribute and I had tears in my eyes afterwards… especially when Matt’s lovely voice came on.”
Another commented: ‘I cried! He meant a lot to me as a chef!’ while another confessed: “Oh damn… I’m leaving again” alongside a crying emoji.
One viewer wrote the lengthy message: “So terribly sad and shocked.” After seeing it on your Christmas show I thought I was in remission.
‘They made cooking together so much fun. Great to see and a fantastic range of recipes to suit everyone. Brilliant chefs. He will be missed. RIP Dave.’
Another added: “I’m so upset and I didn’t even know Dave personally.” I can’t imagine how horrible it must be for his family and friends.
“The fact that it seems like we’ve all lost a friend is testament to how genuinely lovely and authentic Dave was. A very sad loss.”


The television chef died on Wednesday at the age of 66 accompanied by his family and friends, two years after revealing that he was undergoing treatment for an unspecified type of cancer.


Announcing the news, Si wrote: ‘My best friend is on a journey that I cannot continue for now. I will miss him every day and the bond and friendship we shared for half a lifetime’ (the couple in Dave’s last photos in February)


Si also shared this black and white photo of him sitting with Dave on a bench.
Si announced the news of Dave’s sad passing in a heartbreaking statement on Thursday: “Hello everyone, I’m afraid I have some sad news.”
‘Most of you will know that Dave has been battling cancer for the last few years.
‘Last night, February 28, 2024, with Dave’s wife Lili, his family, his close friend David and I at his side, he passed away peacefully at home.
‘Everyone who knew Dave is devastated by his passing. His beloved wife brought him as much happiness as his children, Iza and Sergiu, whom Dave loved as if they were his own.
‘Personally, I’m not sure I can put into words how I feel right now.
‘My best friend is on a journey that I cannot continue for now. I will miss him every day and the bond and friendship we shared for half a lifetime.
‘I wish you the speed of God brother; You are and will continue to be a lighthouse in this world. See you on the other side. I love you.’
