- A scientist trained a system with a data set of 10,000 brain cancer scans
- AI can predict whether a patient will survive eight months after treatment
- Read more: AI develops cancer treatment in just 30 days
Artificial intelligence can predict the survival rate of patients suffering from the deadliest type of cancer, scientists have revealed.
Researchers at King’s College London trained a system to determine whether people diagnosed with glioblastoma would live at least eight months after radiotherapy, allowing doctors to explore other treatments if patients did not.
The median survival time for glioblastoma is 12 to 18 months: only 25 percent of patients survive more than one year and only five percent of patients survive more than five years.
Patients typically need regular scans before doctors can see how effective the drug is, but the new system showed it could provide the same results by analyzing a single MRI.
Researchers at King’s College London trained a system to determine whether individuals diagnosed with glioblastoma would live at least eight months after radiotherapy, allowing doctors to explore other treatments if patients did not.
The AI was trained on a data set of 10,000 MRI scans from different types of cancer.
Alysha Chelliah, who participated in the study, said: “We applied deep learning to predict whether glioblastoma patients will survive the first eight months after completing radiotherapy.
“This approach aims to improve the ability to identify patients who require early second-line treatment or enrollment in a clinical trial, compared to those who show an initial response to treatment.”
The National Cancer Research Foundation, which funds cancer research, says glioblastomas are the “most lethal form of brain cancer.”
It develops when the cells that support nerves in the brain begin to divide uncontrollably.
The fast-growing cells invade nearby brain tissue, making them difficult to remove, but they generally do not spread to other areas of the body.
It is estimated that approximately one in every 30,000 people suffers from this condition.
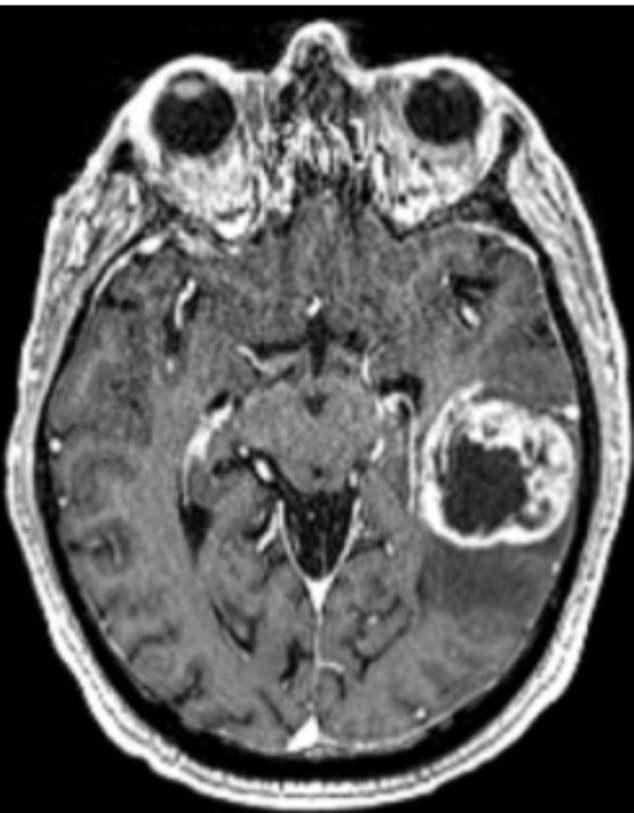
The median survival time for glioblastoma is 12 to 18 months: only 25 percent of patients survive more than one year and only five percent of patients survive more than five years. The black mass in the upper right corner is glioblastoma.
Dr Thomas Booth, who was involved in the research, said: “This study was motivated by a critical and clinically attuned research question about aggressive brain tumours, and was conducted leveraging cutting-edge artificial intelligence.
“Although less common than other cancers, the devastation is disproportionate, with a two-year survival rate of 18 percent.”
The team set out to find a better method for predicting short- and long-term survival rates, which would eliminate the need for multiple scans that can delay treatments.
“Rather than trying to interpret each and every non-specific follow-up brain scan, we simply analyzed a routine scan after radiotherapy and made an accurate prediction using artificial intelligence to answer a simple question: which patients will not survive the next . eight months,” Booth said.
“AI was able to give us immediate and accurate prediction, meaning doctors can empower patients to make decisions about their treatment.”