Two immigrant stowaways who were found hiding in the luggage hold of a school coach were treated with “compassion” by staff and parents and posed “no threat”, the school said today, despite claims that They left the bags covered in urine.
The suspected illegal immigrants were found as children from Hounsdown School in Totton, Hampshire, returned from a trip to France.
The school students, their teachers and their parents waiting to pick them up were stunned when they arrived home after the three-day trip and found the stowaways.
Two men were found hiding among the luggage when the hold was opened after the return journey to the UK.
In a statement, the school said: “Following the statement from Hampshire Police published over the weekend, the school can confirm that two possible illegal immigrants were discovered hiding in the luggage compartment of a coach returning from France on a school trip”.
A school bus returned to Hounsdown School in Totton, Hampshire, on Saturday, but found two unexpected passengers hiding with luggage underneath.

Pictured is Hounsdown School, where the pupils returned after their trip to France.
‘The police attended quickly, although there was no sense of threat to the school community present.
‘The two people found were treated with compassion by staff and parents at all times.
“Investigations into the matter rest with the Home Office, which is working with other agencies as necessary and we therefore have no further comment to make.”
The Home Office has said it will not share any further information about the incident at this time.
A Home Office spokesperson added: ‘The Government works closely with law enforcement agencies to tackle illegal migration in all its forms.
“Our Illegal Migration Bill will mean that people who arrive illegally in the UK will be detained and quickly removed to their country of origin or a safe third country.”
A mother waiting to pick up her son said the incident was “horrible.”
One of the men tried to flee, but was stopped by parents and a child’s luggage was said to be covered in urine.
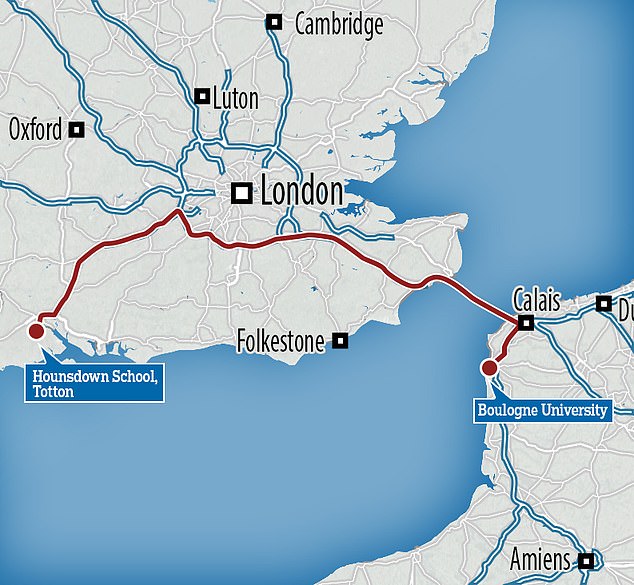
The coach was carrying 9th and 10th graders who had just returned from a three-day school trip to visit the University of Boulogne, about 20 miles south of Calais.
Teachers and pupils returned to Totton, near Southampton, on Saturday afternoon by coach via the Channel Tunnel in Calais.
“It was horrible,” one mother said.
Describing the moment the men were found, she said: ‘(My son’s) luggage was covered in urine and his belongings were crumpled because one of the men was on top of it.
“I asked them (in French) if they spoke English or French and they answered me in French. I was about to ask them where they came from, but the teachers made me leave.”

It comes after 120 migrants crossed the English Channel in small boats on Saturday, bringing the total number of arrivals this year to 1,506. Photographs taken at Dover Docks on Saturday
After the discovery, she panicked and her only thought was to grab her 14-year-old son’s luggage from the bus.
She said: ‘The only way I can describe it is in panic mode.
“My only goal was to get my son off the bus, and once I did that I went back because I couldn’t stand seeing the kids ask them to get their luggage out of the hold.
“I just said ‘excuse me-moi’ to the gentleman and leaned over him to get the rest of the bags out while my son’s was stuffed under him.”
Yesterday a teenager described her surprise at discovering the immigrants in the hold of the bus.
Scarlett Qiunton told ITV Meridian: “We got off the bus and the compartment opened and everyone was trying to grab their bags and then I saw a man sitting at the back.
“He was very calm, he was just sitting there looking at us and seemed quite comfortable, and my friend and I were like, ‘Oh my God, there’s someone there.'”
“The teacher was trying to keep everything calm and just trying to get everyone to go home and obviously do their teacher things, but then I heard someone else in my ear say, ‘oh, there’s two more there.’
“I kind of saw his legs and then I ran to my mother.
“Actually, it was all a shock.”
Scarlett, a Year 9 student, retrieved her suitcase before getting into the car with her mother to return home.
He said that despite the shock, he sympathizes with the people found inside the bus.
“I really can’t blame them,” Scarlett added.
‘They’re probably just trying to get a better life.
“I think it’s important to be respectful because obviously we don’t really know their background and they could come from a war-torn country or something.”
One mother, who had been at the school to pick up her daughter, told the BBC: “I saw a man with his hood up, but I think there were two.”
The woman, identified only as Tabi, added: “They looked to be in their 20s or 30s.”
“My daughter came running and said, ‘Oh my God, there are people sitting where the suitcases are.’
“It’s obviously quite worrying because there were 36 children on the bus and no one knew they were there.
“I understand that these immigrants want a better life, but it’s not very good to target a bus full of children.”
Another parent posted on social media: “Just picked up my daughter from her school trip to France. The bus driver opened the bottom to take out the suitcases and found immigrants sitting there.
Several parents who saw the incident told of their surprise.
“They looked completely fine and comfortable,” one said on social media.
‘It’s not funny, but I’m angry about it. They gained access to a bus carrying schoolchildren.
“It’s one thing to get on a truck and quite another to get on a bus without being seen.”

The Border Force vessel Typhoon carrying migrants arrives at Dover docks on Saturday. One image showed a migrant wrapped in an aluminum blanket being pushed in a wheelchair.
He added: “It was an absolute surprise to see a person sitting there while the children went to get their bags.”
Another parent said: ‘My son is so angry, bless him, he told me to cancel his trip to school next year and said he’d rather wait until he can afford to go when he’s older.’
‘Poor little* too after such an incredible trip! The teachers couldn’t have done a better job throughout the whole process, I really feel for them right now.’
Hampshire Police confirmed officers attended but no arrests were made.
A spokesperson for the force said: “We were called just before 05.15pm on Saturday, February 10, to reports that two people, who were possibly illegal immigrants, had been found at Hounsdown School in Totton.
Agents have attended. No arrests have been made.’

