Democrats in Minnesota are irritated by the “antiquated” law that prevents women from going topless in public after one of them was jailed for 90 days for exposing herself at a gas station.
Eloisa Plancarte, 27, told police that “Catholic girls do it all the time” while being questioned at the Kwik Trip in Rochester in July 2021.
She appealed her conviction, claiming that a man would not have been arrested and that the prosecution violated her constitutional right to equal protection under the law.
Plancarte lost the appeal last month by a narrow 2-1 decision, and Minnesota House Representative Samantha Sencer-Mura has now pledged to change the law.
“This seems really wrong to me,” he said. The star tribune“Particularly now that we, as a society, think differently about gender and gender identity, I think this law seems very outdated.”

Minnesota House Democrat Samantha Sencer-Mura says women should have the same freedom as men to expose their breasts in public without fear of prosecution.


The Representative was moved by the case of Eloisa Plancarte after she was imprisoned for 90 days for indecent exposure at a Rochester gas station.
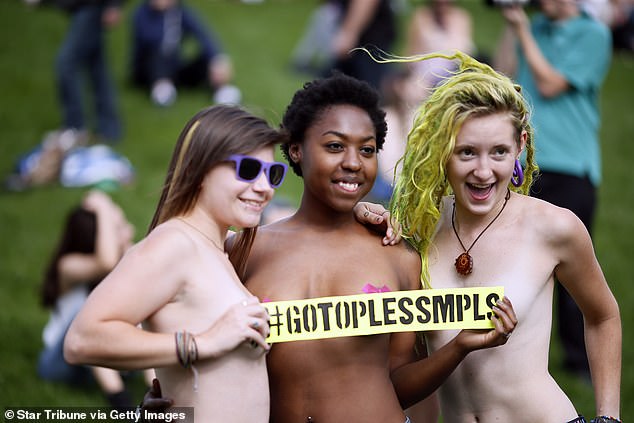
Protests against ‘discriminatory’ indecency laws have been gathering steam for years, including this demonstration in Minnesota in 2015.
Minnesota law defines indecent exposure as an incident in which someone “intentionally and lasciviously exposes the person’s body or private parts.”
But there have been periodic protests both in the United States and abroad that women’s breasts are considered private while men’s are not.
Dissenting Justice Diane B. Bratvold said the decision “raises more questions about criminal conduct than it clarifies,” and that the growing prominence of transgender men and women will likely further complicate matters.
“Each year, viewers of the Academy Awards and New York Fashion Week see a variety of fashions that expose the breasts to varying degrees,” she wrote.
‘How does majority rule apply to a person whose gender identity differs from the sex assigned at birth?
‘Or a person whose breasts have been surgically altered, which happens for a wide variety of reasons?
‘Is a transgender woman who has not physically transitioned her breasts engaging in criminal conduct when she is topless?’
In 2020, the Supreme Court ruled that the prosecution of three women who removed their swimsuit tops on a New Hampshire beach did not violate their constitutional rights.


The Brazilian model was arrested and threatened with a year in prison for taking off her shirt and tying it around her waist while walking her dogs along a beach in Balneario Camboriu last year.


“What should be normal for both genders ends up being denied to one of them in an arbitrary and repressive way,” he said.




Kia Sinclair (left) and Ginger Pierro (right) were arrested in 2016 after taking off their tops on a New Hampshire beach and refusing to put them on when beachgoers complained.
Heidi Lilley, Kia Sinclair and Ginger Pierro were arrested in 2016 after taking off their shirts on a Laconia beach and refusing to put them on when beachgoers complained. Pierro did yoga, while the other two sunbathed.
Brazilian model Caroline Werner, 37, lashed out at the country’s “patriarchal and violent culture” when she was threatened with a year in jail last year after going topless while walking her dog near a beach in the southern city. from Balneário Camboriú.
“Unfortunately, in my country, although the Constitution guarantees equality, in practice this does not happen,” he said.
‘What should be normal for both genders ends up being denied to one of them in an arbitrary and repressive way.’
Chief Justice Kevin G. Ross cited case law dating back nearly 40 years when he upheld Plancarte’s conviction.
“Because a woman’s fully exposed breasts are ‘private parts’ under the statute and intentionally exposing them in a convenience store parking lot constitutes willful and lascivious exposure, we reject her argument of insufficient evidence,” he wrote.
“And since a woman who fully exposes her breasts is not in a similar situation to a man who exposes his breasts, we reject his equal protection argument.”
But Sencer-Mura warned that the issue will not go away and that existing law can no longer address gender ambiguity.
“If authorities believe someone identifies as a woman, then they will treat them differently if they take their shirt off than someone they perceive as a man,” he said.
“As we have a changing understanding of gender, that law no longer makes sense.”
