Another week, another deliciously fun reality show follows women with too much time and money on their hands.
Married To The Game is about to launch on Amazon Prime and it’s a world that I, as a former WAG, know very well.
The series follows the latest glut of wives and female partners who have joined forces with a top footballer. However, amidst the excessive lifestyles, hair, handbags and OTT homes, everyone is at pains to point out that their world is not as good as it seems.
A clip lamenting the trials and tribulations of the series’ endless designer bags and first-class travel has gone viral, and no wonder!
Taylor Ward, 26, a gorgeous glamor blonde with 2.8 million Instagram followers and collaborations with everything from hair straighteners to nail kits, is catnip for the cameras flying on the wall.
In the cleverly cut trailer she is seen breaking down in tears as her husband Riyad Mahrez, 32, bluntly tells her he is moving Manchester City teams to Saudi Arabia in a lucrative deal worth £750,000 a week. When she shouts, “I’m going to stay home alone,” Riyad responds, “It’s part of the game, no.”
Taylor Ward cries after her husband Riyad Mahrez told her they were moving to Saudi Arabia in the Married To The Game trailer.

Speaking to the former Manchester City player, 32, on a new reality TV show, Married To The Game, she said: “I’m going to stay home alone,” to which Riyad replied: “It’s part of the game it can’t be done

Lizzie Cundy was married to Premier League star Jason for 16 years

Ward and Mahrez celebrate Manchester City’s Champions League victory last year
This WAG, for example, is Team Riyad. I moved four times in five years when I was married to former Chelsea player Jason Cundy. I had been notified more often when my personal trainer changed an appointment than some of my ex-husband’s club transfers.
In the first episode of the six-part show, premiering this Friday, February 23, we’re in the spacious dressing room of Taylor’s Cheshire mansion as she chats to fellow WAG Sara Gundogan, 29, who is married to the former Manchester City player Ilkay. Gundogan. Taylor’s 18-month-old daughter Mila is casually given several designer bags, including a black quilted Chanel clutch and a Louis Vuitton model, for her to play with. When Taylor announces that she has always lived in Manchester and that her ‘biggest fear is moving’… Well, we know what’s coming, right?
Footage from July 2023 of Franco-Algerian Riyad’s much-hyped move to Saudi Arabian club Al-Ahli is used to announce his £30m transfer alongside clips of Taylor, a former model, driving her Mercedes 4×4 G-Class SUV. six figures down an elegant country road while complaining, without any irony, that the measure was a “shock for everyone” and how “football is brutal.”
Sorry, Taylor, but you can’t go down the “poor me” route when you’re a WAG; you really have to take the “hold on to the buttercup” approach to life.
While you may have the high-end interiors just the way you like them, the kids in the best schools and you’ve finally discovered the perfect nail salon, a transfer deal can be finalized in a matter of hours and you should be prepared to leave in a blink of an eye. This is part of the deal and, let’s face it, what funds your lavish lifestyle.
I get it: you don’t know anyone in the new destination, much less know how to speak the slang. And Saudi Arabia is hardly known for its liberal women’s rights.
In a scene after modeling jewelry with her sister, Taylor cries about her impending move to Saudi Arabia and complains, “If I don’t like it, I have no choice.”
I get it, Taylor! You’ve got the cars, the clothes, the Cheshire mansion, the private jet and the permanent tan… but having your custom-made silk rug taken away while you start a new life thousands of miles from home is going to help you feel very only.
Especially if you go the “pity me” route.
In addition to Taylor and Sara, the first episode introduces Cat Harding, fiancée of Arsenal player Jorginho (and mother of one of Jude Law’s seven children).
Cat, 33, a former contestant on ITV’s The Voice UK, decides to throw her own birthday party, complete with a white baby grand piano, carnival dancers and harpists. The (somewhat exhausted) organizer lists some of the last-minute changes she insists on, including an entrance with balloons and 65kg of lemons.
We cringe when Cat asks her Brazilian boyfriend Jorginho if she should leave her ring finger free for a proposal… The answer is a resounding ‘no’! (The couple finally got engaged in December under a neon “will you marry me?” sign inside a heart made of flowers.)
We also see Sara sigh on camera when her husband Gundogan, 33, is transferred to Barcelona: “You just get a call and you get informed… it changes your life.”
She stayed in Manchester packing his suitcase, with his framed shirts hanging on the wall behind her. And what do you want Sara to take by plane? Hers ‘two treatment tables’ of hers (and that’s after telling viewers that he only trusts his mother to pack his bags for him).

Arsenal’s Jorginho is cheered on by his fiancee Cat Harding (pictured), star of the show.
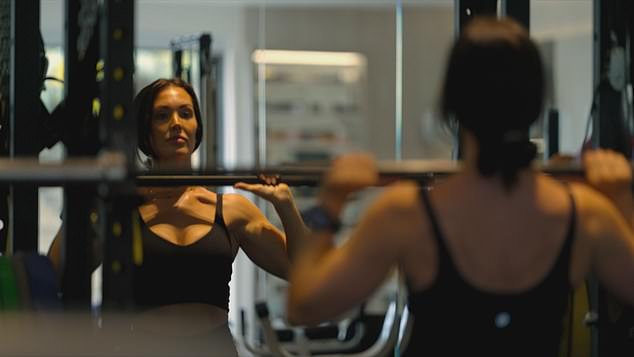
Married To The Game follows Samantha, the wife of Everton centre-back James Tarkowski, on her journey to opening her own gym, having gained personal training qualifications.
There is nothing worse for a footballer than a wife who moans and moans. This is difficult advice to give, but my words of wisdom to people like Taylor, Cat, Sara and their generation are this: club moves are the bread and butter of life as a footballer; It is never a given that the club shirt they wear this week is the same one they will wear next season.
You have to be incredibly naive if you assume your husband will start and finish his career in the same zip code. I’m sorry to tell you, loves, but that’s simply not how The Game works.
When you say ‘I do’ you are also committing to your life as a footballer and everything that entails.
Look at Victoria Beckham. Despite being at the peak of her career as a Spice Girl, she circled the planet to follow David. She learned her lesson early after making the silly mistake of staying in Blighty during David’s move to Real Madrid in 2003, when her alleged four-month affair with her personal assistant Rebecca Loos took place.
No wonder Victoria quickly uprooted her life to follow him to Los Angeles in 2007.
That’s why I cringed when, at the end of the first episode, a wide-eyed Taylor says, “I don’t know when I’ll see it again, which is pretty sad.”
By then her husband was already settled in Saudi Arabia.
Look, a five-year deal in a Middle Eastern country isn’t exactly a happy ending, is it? But seeing the person you love playing world-class soccer in a stadium with more than 70,000 fans chanting his name means he’s routinely treated like a world-class handsome man; That adulation is greater than that of a rock star because football is global. When he does well, you get a little bit of that stardust too. You feel special when the world rolls out the red carpet.
That’s why being the wife of a footballer is so attractive. That is why young women see this lifestyle as something accessible. They can’t be Jennifer Anniston or Angelina Jolie, but could they be the next Coleen Rooney or Rebekah Vardy? With enough hair extensions, fake tan, and cleavage, you can bet. There are clubs all over the country with bars and nightclubs packed with footballers. And the reality is that if you look good it is very easy to catch one.
That’s not to say, of course, that there aren’t downsides to being a WAG, and I’m proof of that.
There is the constant threat of other women trying to take your place in the bedroom. Never forget that, apart from those weekly games, footballers train in the morning, do a bit of physio and then have a lot of free time. A young man, with a fit body and a lot of dosh who believes he is invincible, is a green light for any woman with a pulse.
And as for those wives with their heads in the clouds who think that staying in the comfort of their home in Blighty is the best option for them and the children, I have this to say: big mistake.
I know very well the dangers of the WAG world. Jason and I split up when I found out he was dating a younger woman in 2010. We had been married for 16 years and had two children, who were ten and 16 at the time. But despite a lifetime of vigilance, I couldn’t stop it from happening. .
I know a WAG who told her other half when she was transferred overseas: “I’m happy in Surrey, I’m not going.” Choosing Cobham over the club move was unwise. Quelle surprise: they separated two months later. The job of a footballer’s wife is to support her husband. She may be married to him, but her first love will always be the game.
People like Taylor need to focus on her husband’s happiness. Believe me, if he is happy, you will be too.
So my advice would be: WAG, when you get transferred to another country, dry those tears, stop complaining and move on. This is the life he (and you) have signed up for.
As told to Samantha Brick
- The docu-series Married to The Game launches on Prime Video on Friday, February 23.

