A second case of measles has been confirmed at a migrant shelter in Chicago, marking the first cases in the state in five years and highlighting the public health risk posed by overcrowded migrant housing.
The Chicago Department of Public Health confirmed the second case Sunday and said the patient is hospitalized but stable.
As millions of migrants have come to America under President Joe Biden’s immigration policies, experts have warned that overcrowded shelters and low vaccination rates in other countries could leave the United States vulnerable to disease outbreaks.
They have said that asylum seekers can bring infectious diseases across the southern border and “open border” policies lead to drug-resistant diseases.
And city leaders have said migrants are arriving in their areas in ‘disturbing’ and ‘very very unhealthy’ conditions.
Migrants themselves have said that diseases are rampant in shelters due to overcrowding and unsanitary conditions.
Chicago’s latest outbreak adds to a growing list across the country that has seen clusters of tuberculosis, chickenpox and an unidentified disease that killed a five-year-old boy in December.

Dozens of migrant families are seen arriving from Texas at the Port Authority Bus Terminal in New York in September 2023
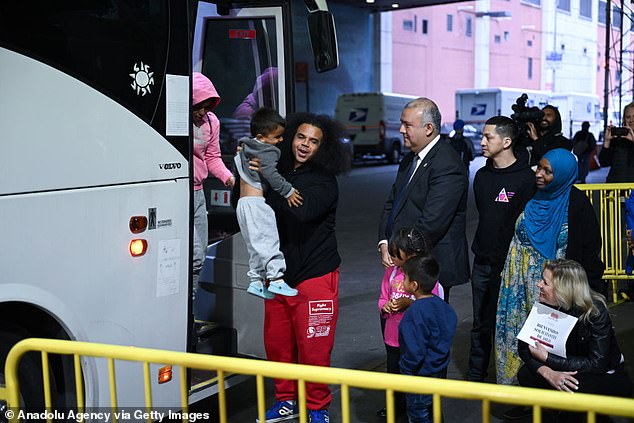
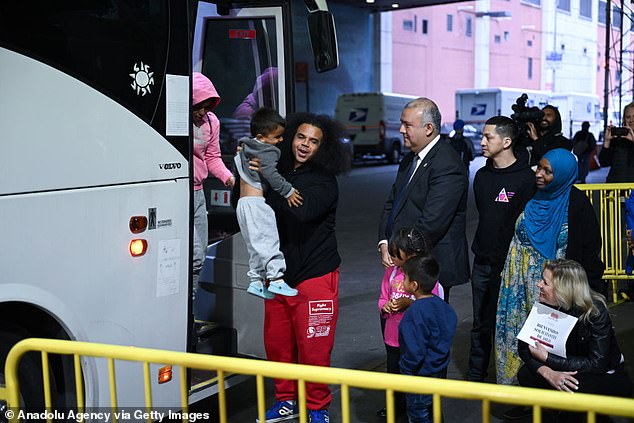
A bus carrying migrants from Texas arrives at the Port Authority bus station in New York, USA on May 3, 2023
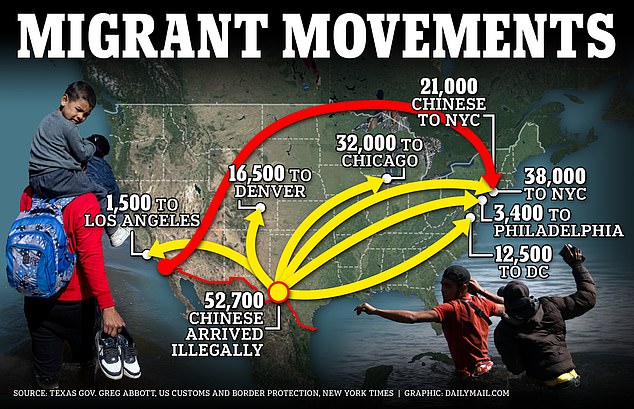

Texas has bused more than 105,000 migrants to sanctuary cities since 2022, according to governor’s office
In April 2023, New York City Health Commissioner Ashwin Vasan urged officials and doctors to take extra care when treating or screening migrants to prevent a public health crisis—noting that many do not have routine vaccinations.
In fact, he said, 50 percent of the migrants going to New York City did not have their polio vaccine.
Dr. Marc Siegel, medical director at New York University, wrote for USA Today: ‘Migrants may bring infectious diseases across our southern border. When they go by bus to New York and other places, these diseases come with them.’
And Dr. James Hodges, an internist who practices on the Texas border, told the publication that the ‘open border’ is leading to more drug-resistant tuberculosis (TB) in the US.
The CDC requires all immigrants and refugees to undergo a medical screening before entering the United States that includes a brief physical exam, a mental health evaluation, review of vaccination records, testing for STIs, and a tuberculosis screening.
Immigration applicants with communicable diseases are not allowed to enter the United States, but not all go through the proper channels, meaning migrants who are sick can slip through the cracks and bring disease with them.
Over the past 18 months, Chicago has welcomed more than 36,600 migrants — with the majority from Venezuela, which has recently battled measles outbreaks and has a low vaccination rate.
And Chicago’s migrant housing center has been involved in several previous outbreaks, including one that left a five-year-old dead.
In December 2023, the boy was a resident of a shelter meant to house 1,000 people, but held about 2,400 at the time.
Witnesses at the shelter said the boy had a temperature over 100 degrees Fahrenheit and was convulsing and bleeding from the mouth and nose. Officials said he later died at the hospital, but witnesses report he died at the shelter.
In the same week, six other residents were hospitalized with unspecified illnesses.
Residents of the shelter told The Chicago Sun Times reported that diseases were spreading in the homes due to overcrowding and unsanitary conditions.
Associated Press reportedciting people living at the overcrowded facility that there was faulty heat, water leaks, expired food and overcrowded conditions.
At the time, Chicago Mayor Brandon Johnson blamed border cities for the outbreak, saying migrants were arriving in Chicago under conditions that “are pretty disturbing.”
He told reporters: ‘People turn up in very extreme circumstances. Very very unhealthy.
‘They just drop people off anywhere. Do you understand how uneven and how bad it is?’
New York City, which has seen more than 157,600 migrants arrive since spring 2022, was battling a tuberculosis outbreak that some health experts attributed in part to the influx.
In Dr. Vasan’s letter from 2023, he specifically named tuberculosis as a disease of concern.
Last autumn, the five boroughs recorded a ‘dramatic’ rise in cases of tuberculosis, once one of the deadliest infections in the world – and a death sentence for half of those infected.
But with the advent of vaccines, which are up to 80 percent effective in preventing serious disease, the death rate has fallen to less than four percent in developed countries.
In 2023, the city saw more than 500 cases of tuberculosis—a 20 percent increase from 2022.
While some health officials said the increase was due to the Covid pandemic hindering the diagnosis and treatment of TB, others speculated that the increase could have been from the increase of migrants, who are at an increased risk of infection because the disease can easily spread in the types of crowded, mundane surroundings in which they are housed.
Dr. Vasan wrote: ‘Many people who recently arrived in NYC have lived in or traveled through countries with high rates of TB.’
In Denver, several cases of chickenpox were reported among children in the city’s migrant shelters in November. City health officials said they treated the children and began vaccinating people in the migrant population.
In his letter, Dr. Vasan that vaccinating migrants, as well as screening them for disease, should be a top priority.
