Table of Contents
While most scientists look to the stars for signs of extraterrestrial life, others say the evidence could already be here on Earth.
This week mysterious remains surfaced in Colombia, which some say could have their origins beyond this world.
Veteran public radio reporter Josep Guijarro said the unusual corpse could be an alien or a “small humanoid” from an ancient species.
But experts now say the real explanation is probably much simpler.
Professor Sian Halcrow, a forensic anthropologist and expert in infant remains, told MailOnline that these are probably the remains of a premature human baby.
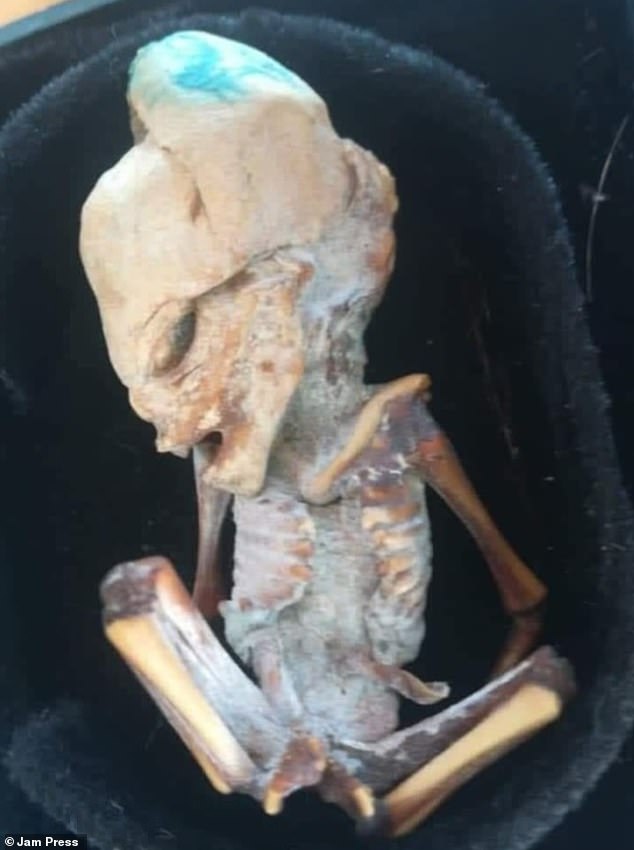
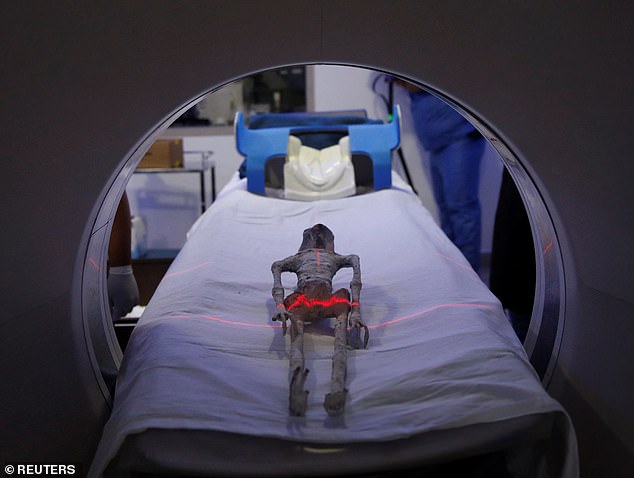
These strange images of an ‘alien fetus’ were shared by former public radio host and extraterrestrial researcher Josep Guijarro.
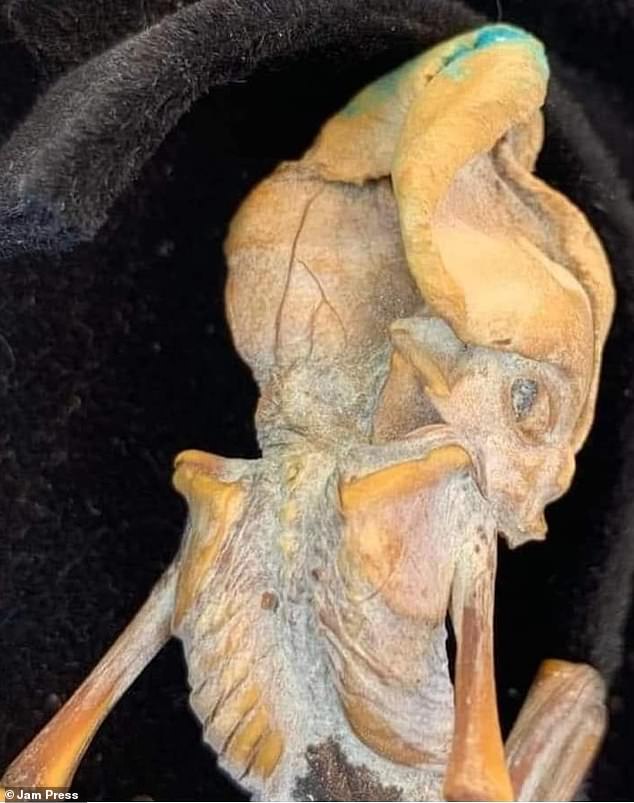

These remains appear to have extraterrestrial characteristics, but experts suggest they are consistent with the appearance of mummified human fetuses.
What is claimed?
These strange images were shared by veteran public radio host Josep Guijarro, who is now a full-time extraterrestrial researcher.
According to Guijarro, the images were shared with him by a source who “wanted to know if it could be a being from another world and informed me that the specimen comes from Colombia.”
The alleged alien has a large, elongated skull, slanted eyes, an umbilical cord and an “unusual number of ribs.”
In an article published in Mystery Space, He stated that the remains only had 10 ribs on each side of the body compared to 12 in the typical human.
Guijarro also claims that the remains emerged from ‘el cerro de los enanos’ (‘el Cerro de los Enanos’) in remote Colombia.
However, in a later post about X, he added that he could not know the exact origin of the specimen because it lacked “verifiable data.”
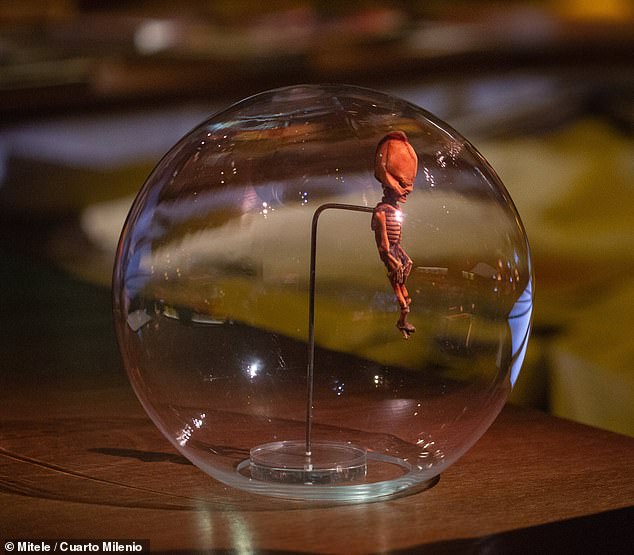
The new find resembles the mysterious oblong-headed ‘Atacama skeleton’ from Chile (above), which according to a Spanish businessman who spent a decade studying it, may have once been a small kind of terrestrial humanoid.
The publication has sparked a wave of speculation online that these remains could be those of an extraterrestrial species that arrived on Earth at some point in the distant past.
One social media commenter wrote: ‘Surely it’s an intraterrestrial species still living among us?’
These claims echo theories surrounding “alien mummies” that were presented to Mexico’s Congress last September.
However, those claims were soon refuted when analysis revealed that the “aliens” were nothing more than dolls made of animal bones.
However, Guijarro has tried to distance himself from these theories and has proposed an alternative, although still far-fetched, suggestion.
In an apparent dig at the Mexican alien debacle, he wrote: “I’m sure someone in Mexico would have already given it the ‘alien’ label, but in my case I prefer to be more cautious.”
Instead, pointing out the “non-trivial detail” of the umbilical cord, Guijarros suggests that these remains are those of an ancient species of “tiny humanoid.”
The Spanish public radio veteran ventured to suggest that the specimen could be related to ‘Ata’, an infamous six-inch ‘alien’-like corpse unearthed in Chile in 2003.
It suggests that both specimens could be related members of a species of human-like creatures that lived about 800 years ago.
“The legends speak of a civilization of tiny beings, about 35-40 centimeters, who would live on the top of these mountains,” he wrote.


Guijarro’s skepticism has not prevented others from weighing in with their own theories about the new mystery of the Colombian corpse. “It’s very similar to the Atacama being,” said one (above). ‘Surely it is an intraterrestrial species that still lives among us?’

The ‘aliens’ presented to Mexico’s Congress in September were revealed to be nothing more than human-made bone dolls.
What do the experts say?
However, despite online speculation, expert opinion suggests a much simpler explanation.
Professor Halcrow told MailOnline that all the alleged evidence for the specimen’s extraterrestrial origin could be easily explained.
She said: “There are always conspiracy theories and unfortunately some people pick them up because they are the most sensational and get the most attention.”
“However, they have ignored the most parsimonious explanation: that it is a premature baby.”
The unusual appearance of the remains is due to mummification of soft tissues in arid conditions, according to Professor Halcrow.
Since fetuses have softer bones and are not fully developed, this mummification process can make the remains appear unusual to unfamiliar observers.
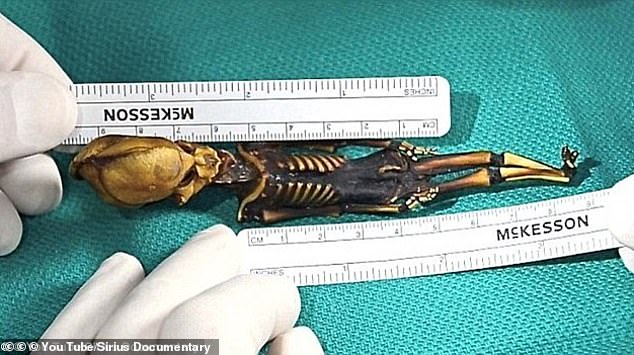

Previous ‘aliens’ and tiny humanoids (pictured) have been studied by experts and all have common characteristics that can be explained by soft tissue mummification in fetuses or premature babies.
Professor Halcrow explained: ‘The anatomy of this individual is consistent with that of a mummified human fetus.
“The misshapen appearance of the skull may be due to molding of the fetal head during birth, where the parietal bone (large bones on either side and at the top of the skull) may overlap the frontal bones and other parietal bones.”
Likewise, this theory may also explain the “alien” characteristics that are evident in the mummy.
“Babies only open their eyes in utero at around 27 weeks’ gestation, so the suspected eye malformations are the result of mummification of the soft tissues of the eyes and eyelids,” Professor Halcrow said.
As for the claim that there are only 10 ribs on each side, Professor Halcrow says there is “no reason” to believe this is the case.
Since the lower two ribs are very small, they are extremely difficult to see and would be difficult to detect from imaging alone.
More worryingly, Professor Halcrow also points out that Guijarros does not mention the context in which these remains were found.
And he added: ‘It is mentioned that it is from 800 years ago. If that’s the case, this baby comes from an old looted cemetery.
