Phrases like “like father, like son” suggest that it is not just appearances that are passed down from generation to generation.
In fact, we are commonly led to believe that personality traits are inherited from our mom or dad.
But a new study claims there may actually be little truth to this.
Researchers at the University of Edinburgh say we are slightly more likely to share personality traits with our parents than with a random stranger.
They report that it is “impossible to accurately predict a child’s personality traits from those of his mother or father.”
Like father Like Son? Experts say it’s “impossible” to accurately predict a child’s personality traits from those of their parents.
“In almost every language there is a form of the English proverb ‘like son, like son,'” lead author Dr René Mottus, from the University of Edinburgh, told MailOnline.
‘Many people believe this and sometimes make judgments about people based on their parents.
‘But it turns out that this proverb is not very accurate when it comes to personality traits: our habitual patterns of thinking, feeling and behaving.
“There’s a small chance that people are more like their parents than any random stranger.”
Working with experts from the University of Tartu, Estonia, Dr. Mottus and his colleagues recruited more than 1,000 family pairs from the Estonian Biobank, a large collection of health information from volunteers in the country.
Participants reported their own levels of the “Big Five” traits—openness, conscientiousness, extraversion, agreeableness, and neuroticism—as well as life satisfaction.
The “Big Five” personality traits are the best accepted and most widely used personality model in academic psychology.
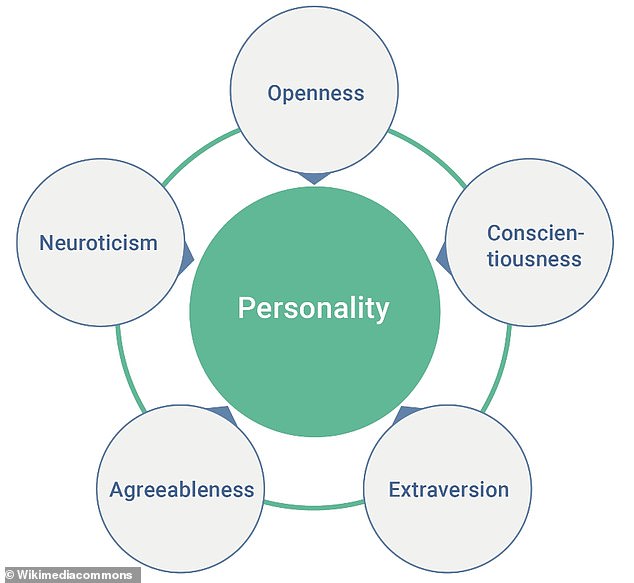
The ‘Big Five’ personality traits are the best accepted and most widely used personality model in academic psychology.
Each person rated their own personality traits, but to get more accurate results, the researchers got a second opinion from an “informant,” usually their partner.
“Self-ratings alone aren’t very reliable, but when two people agree on someone’s traits, they have to take something into account,” Dr. Mottus said.
The results put the heritability of personality traits and life satisfaction at around 40 percent.
Although this is higher than the 25 percent typical in self-report studies, it is not high enough to suggest that we are more likely to share personality traits with parents than with a random stranger.
The experts further explain their findings with a hypothetical scenario.
Suppose a group of parents and their adult children completed a personality test and were placed in the bottom, middle, or top third of the population based on their results.
In this scenario, only 39 percent of the offspring would receive feedback like their parents on any given trait, compared to 33 percent from random strangers.
In other words, more than 60 percent of children belong to a different group than their parents on any given personality trait.
Dr. Mottus emphasizes that the findings “do not mean that personality traits are not heritable at all,” but rather that this heritability is not significant.
What’s more, they are most likely inherited through genes (“nature”) rather than through upbringing (“nurture”).
“By the most precise estimates, around two-thirds of the reasons why people have different personality traits have something to do with their genes,” he told MailOnline.
«But this is not enough for parents and children to be much more similar than strangers.

Common phrases such as “like father, like son” or “like mother, like daughter” suggest that it is not just appearances that are passed down from generation to generation (file photo)
“Furthermore, there is no evidence that the experiences that come with sharing a family make people more alike.
“For example, there is no evidence that adoption into a family makes people’s personality traits similar to those of their adoptive parents or other children in the family.”
The exact origin of our personality has long been a source of fascination for psychologists.
The theory that they are passed from parents to children, either through genes or external factors, is officially known as “family transmission.”
Any similarity between father and son may be responsible for reinforcing the notion that family transmission really exists, along with proverbs like “like father, like son” or “like mother, like daughter.”
“Similar proverbs also exist in many other languages, presumably because they are based on simple and abundant real-world observations,” the team says.
“And yet these proverbs may exaggerate the magnitude of familial transmission, since current data suggest that, on average, parents and children differ only slightly less than strangers.”
The study has been published as a preprint in the PsyArXiv server, meaning it has not yet been peer reviewed.

