The BBC has defended its decision to replace an actress with AI in an upcoming documentary, revealing that the technology has been used to “recreate a voice” for a person who is “approaching the end of life.”
Sara Poyzer, who starred as the lead actress in Mama Mia, raised concerns in the industry after she revealed that the BBC was using an AI voice instead of her in a show.
She posted on social media how she had been informed she was no longer needed for a position as a result of technology.
But this morning the BBC responded to criticism of the decision, which has sparked concern in the acting community.
In a statement, the corporation said it was conducting a “highly sensitive” program with an employee who “cannot speak.”
He added that he had been working with the family on how to represent their voice “when the words they have written are read” at the end of the film.

Sara Poyzer (pictured as Donna Sheridan in Mamma Mia) has dominated the West End for her performance as the lead actress in Mamma Mia for over ten years.

Yesterday she received an email from the corporation telling her that she was no longer needed for a position.
The BBC said that in these “very particular circumstances” and “taking into account the family’s wishes” it had agreed to use AI “for a short section” to “recreate a voice” that could no longer be heard.
A spokesperson said the use of the technology would be “clearly labeled” in the film.
A BBC spokesman said: “We are making a very sensitive documentary featuring a contributor who is approaching the end of his life and is now unable to speak.”
‘We have been working closely with his family to explore how we could better represent the contributor’s voice at the end of the film when the words they have written are read.
‘In these very particular circumstances and taking into account the family’s wishes, we have agreed to use AI for a short section to recreate a voice that can now no longer be heard. This will be clearly labeled within the film.”
Ms. Poyzer has traveled the world playing Donna Sheridan in the musical Mamma Mia for 11 years and has had a successful career as an actress and broadcaster.
He recently starred in the Olivier Award-winning West End show Come From Away and has worked for the BBC for at least 20 years working on the hit shows Doctors, EastEnders and The Archers.
But earlier this week she received an email from the corporation telling her she was no longer needed for that position.


The BBC has decided that a robot can do its job better after replacing actress Sara Poyzer with Artificial Intelligence (File image)


She was inundated with support and many industry professionals said the same thing had happened to them recently.
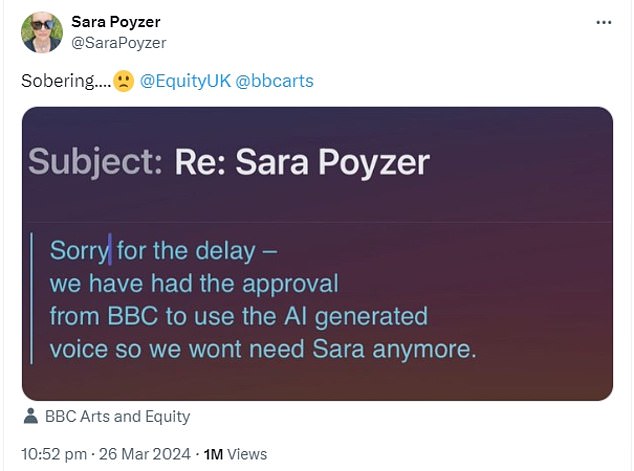
Posting a screenshot on her Twitter and Instagram, the email said: “Sorry for the delay, we’ve had approval from the BBC to use the AI-generated voice so we won’t need Sara anymore.”
Tagging the BBC and the Equity union, Ms Poyzer captioned the photo “sobering…” with a sad face emoji.
The Mail learned that the email was a response from a production company that was working with the BBC on a project hoping to hire Ms Poyzer.
Ms Poyzer was waiting to hear back about whether it had been confirmed, but was told they would use AI instead.
She commented on her post saying that the industry was going through “dark times.”
The BBC’s recently published principles on the use of AI say: “We will always prioritize talent and creativity – no technology can replicate or replace human creativity.”
‘We will always prioritize and reward authentic human storytelling from reporters, writers and broadcasters who are the best in their fields.
‘We will work with them to explore how they could use generative AI to help them push new boundaries. Creators and suppliers play a vital role in our industry. “The BBC will always take into account the rights of artists and rights holders when using generative AI.”


Posting a screenshot on her Twitter and Instagram, the email said: “Sorry for the delay, we’ve had approval from the BBC to use the AI-generated voice so we won’t need Sara anymore.”


Ms Poyzer was waiting to hear back about whether it had been confirmed, but was told they would use AI instead.
Ms Poyzer was inundated with support in the comments and many industry professionals said the same thing had happened to them recently.
“It’s happened to me and art projects many times, I’m sorry this happened to you,” one person said.
Another commented: ‘It happens to all our industries. It’s killing all our jobs. The other day I saw a complete set that was AI.’
“This is horrible and so heartless,” said another.
Equity, the performing arts workers union, launched ‘Stop AI Stealing The Show’ in 2022, a campaign around performers’ rights over artificial intelligence.
The BBC covered and supported the campaign, discussing it intensively on sites such as Front Row and BBC News.
This week the BBC promised to stop using AI to promote Doctor Who after receiving complaints from viewers.
Voice Squad, a voice-over agency working with Ms Poyzer, said: “We were very disappointed to receive the response from the production company, especially as it is a BBC project.
‘The BBC has always opted for quality in its broadcasts of events and dramas. As a voice-over agency, we believe that AI is a danger to the entire industry: it eliminates the work of artists who have trained for three years at a theater school and have spent many years honing their craft.
“Announcers are especially skilled actors who deserve not to have their work devalued.”
The BBC was contacted for comment, while Poyzer declined to comment.
