An interactive map has revealed for the first time the US counties where hearing loss is most common, yielding surprising results.
Contrary to popular belief, it shows that people living in rural areas are up to twice as likely to suffer from hearing loss as their fellow Americans living in urban areas.
The study estimated that in rural areas of New Mexico, Texas and Oregon, up to one in three people five years old or older had this condition, which is diagnosed when someone has difficulty hearing quieter sounds, such as rustling leaves and rustling. buzzing of mosquitoes.
Researchers at the University of Chicago believe that rural Americans are more likely to be exposed to loud noises from farm equipment and firearms, which could damage their hearing.
This comes despite previous research indicating that up to nine in ten city dwellers are at risk of hearing loss due to high volumes of traffic, bars and clubs.
Your browser does not support iframes.
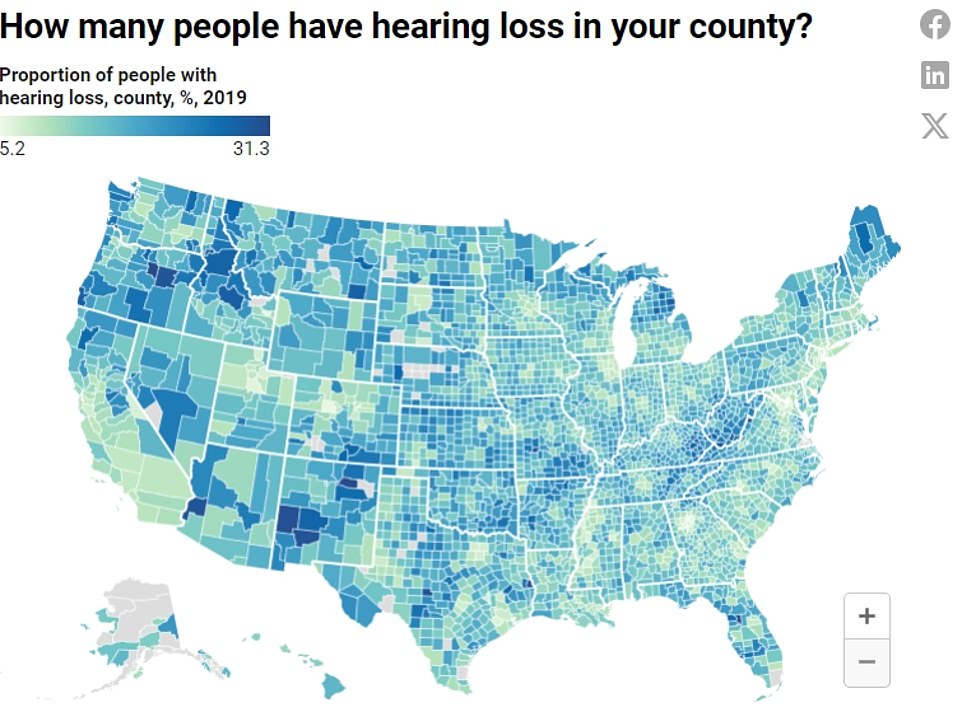
The map above shows the proportion of people estimated to have hearing loss by county.
They cautioned that overall, their study, based on data from 2015 to 2018, showed that hearing loss is a widespread problem in the U.S., and that older men are more likely to suffer from the condition.
Studies suggest that people with this condition are more likely to be depressed and suffer from falls and cognitive impairment, which is related to their inability to hear others and small sounds clearly.
The study used a mathematical model that was based on hearing loss data from the CDC’s annual survey conducted from 2015 to 2018. It was compared to 2019 population estimates.
The National Health and Nutrition Examination Survey (NHANES) interviews a nationally representative sample of 7,000 people each year about their health, including whether they have hearing loss.
Dr David Rein, a public health expert who led the study, and others wrote in the paper: ‘The results of our model suggest that those living in rural areas experience higher rates of hearing loss.
“(This is) perhaps due to potential exposure to noise from work and outdoor recreation, such as forestry, off-road vehicles, and recreational firearms.”
Hearing loss is defined as not being able to hear as well as someone with normal hearing, or sounds up to a threshold of 20 decibels or more in both ears.
Sounds at 20 decibels include the rustling of leaves or the buzzing of a mosquito.
The condition is diagnosed using a test in which sounds and words are directed through headphones to each ear and the patient is then asked to say what they heard.
Hearing loss can be treated through the use of hearing aids, although these are often expensive (up to $3,500 per ear out of pocket), leading many patients to leave the condition untreated.
In the 3,143 counties that make up the United States, the model suggested that Mora County in New Mexico had the worst hearing loss in the country: 31.3 percent of adults had hearing problems.
Florida’s Sumter County, a rural area outside Orlando, also ranked first with 31.3 percent of adults experiencing hearing loss.
Only about 4,100 people live in Mora County, whose largest city, Wagon Mound, is populated by only 265 people. The area is largely made up of farms.


The image above is of the exterior of the largest settlement in Mora County, New Mexico. It is estimated that one in three adults suffers from hearing loss in this area.
Sumter County, on the other hand, has a population of 135,000 people, largely tied to the new development areas being built in the north of the county.
However, most of the area is also made up of farms and agricultural land.
Broken down by state, West Virginia had the highest levels of hearing loss in the country: an estimated 18.2 percent of residents have the problem.
Maine had the second highest level, at 16.2 percent, according to estimates, and Montana had the third highest, at 15.4 percent.
Revealing the data, Dr. Rein added axios: ‘Hearing loss is a problem everywhere.
‘Even if you look at places like Washington DC, where the prevalence is the lowest of any metropolitan county area, we’re still talking about almost 400,000 people with hearing loss.
“It’s something that affects all groups and affects all of us as we get older.”
